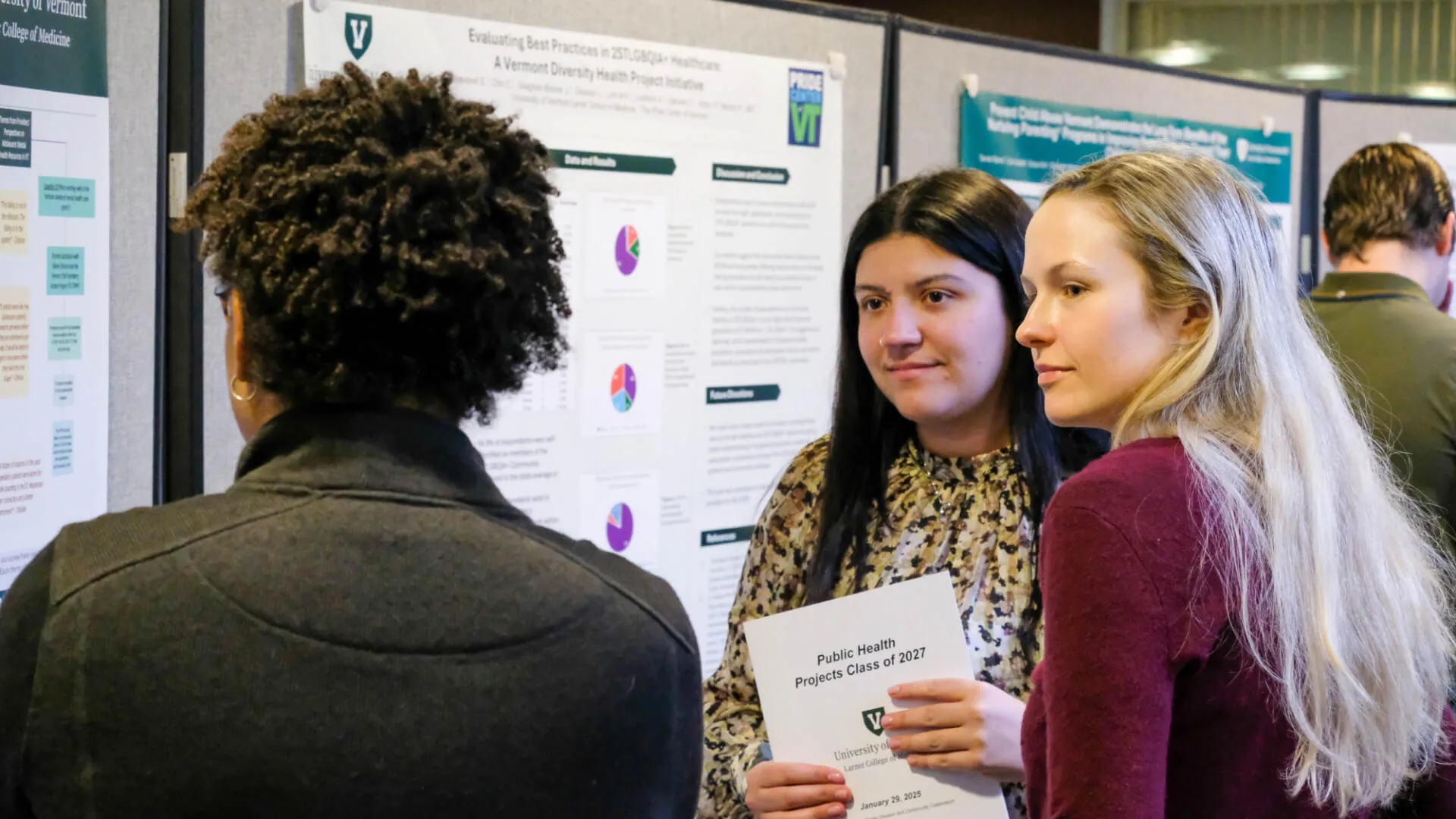
If you’re committed to improving health outcomes for everyone and are passionate about enhancing health access, then the field of Public Health needs you. Explore our Graduate Programs and Certificates to learn how a future in Public Health will work for you!
Meet MPH Student Samantha Collins
Public Health & You
- 1791 university founded
- R1 Top Tier Research University (Carnegie classification)
- 459 acres main campus
Larner College News

Larner Faculty to Lead Largest U.S. Medical Specialty Organization
Public Health Student Award Winners Announced

WVNY-TV Notes Payne Testimony on Primary Care

Public Health in Practice: MPH Students Present Culminating Research at 2026 UVM Student Research Poster Session.

UVM Larner College of Medicine to Launch New Online Doctor of Public Health Program in Fall 2026
Unparalleled Teaching and Expertise
Through groundbreaking research and hands-on fieldwork, our UVM Larner College of Medicine instructors bring unparalleled expertise to the classroom and learning environment.